Everything You Need to Know About Vaginitis

Your vagina is a biome with a balance between bacteria and yeast to help keep it moist and healthy. When your vagina gets irritated or inflamed, it’s called vaginitis, which can be caused by an overgrowth of bacteria or yeast, or another reason. Here’s plain talk about vaginal inflammation to help answer some common questions.
What is Vaginitis?
Broadly, vaginitis is any inflammation of the vagina. The vagina becomes inflamed when the typical balance of yeast and bacteria is disrupted. Vaginitis is very common! Most women and people with vaginas will get vaginitis at least once on their lives for one reason or another. You can get vaginitis at any age, whether or not you’re sexually active.
Vaginitis also causes irritation of the vulva, so it’s sometimes referred to as vulvovaginitis. Some mild vaginitis can resolve itself as your vagina self-corrects, but often you need something to help soothe or restore balance. Over-the-counter creams, vaginal suppositories, and gels can help with discomfort, or your doctor can provide prescriptions to treat infection and vaginitis symptoms.
What Causes Vaginitis?
If you’re wondering how you get vaginitis, it can be caused by:
- An infection, such as from yeast, bacteria, or a parasite.
- Taking antibiotics.
- Hormone changes, such as from menstruation, pregnancy, perimenopause, and menopause.
- Irritation from douches, soaps, or fragrances.
- Spermicides.
- Certain medications that affect the vaginal biome.
- Vaginal dryness.
- A sexually transmitted infection (STI).
The symptoms of vaginitis are basically the same, no matter the cause, so it’s best to see your doctor to determine the root of the inflammation and to get the proper treatment.
What are Vaginitis Symptoms?
Vaginitis can be uncomfortable. If you’re feeling any of these symptoms down there, you could have a form of vaginitis:
- Itching, burning, or irritation.
- A change in the color, smell, or amount of your vaginal discharge.
- Painful sex.
- Painful urination.
- Light bleeding or spotting.
- No symptoms. You might not have any noticeable symptoms or think it’s just a normal way for a vagina to feel. This is another good reason for annual check-ups with your doctor!.
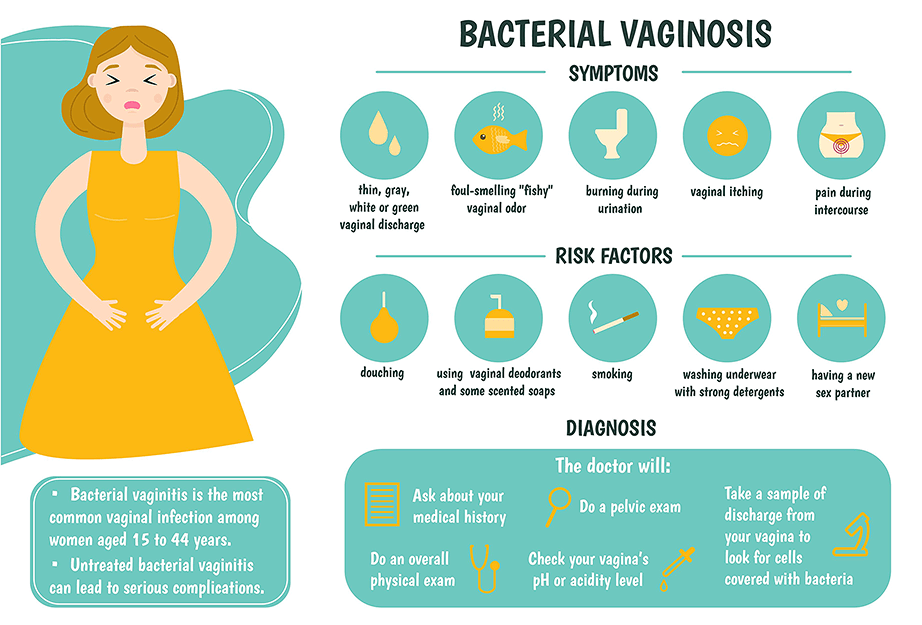
What is the Difference Between Vaginitis and Vaginosis?
Vaginitis is the broader term for any inflammation of the vagina, while vaginosis refers to an infection of the vagina (which causes inflammation). All vaginosis is vaginitis but not all vaginitis is vaginosis. Your doctor can help you learn if your vaginitis is an infection that needs medication.
What are the Types of Vaginitis or Vaginosis?
There are a few types of vaginitis or vaginosis, depending on the root cause. The symptoms are similar, though the amount, color, and odor of your discharge can be different. Here are the basics.
1. Mild vaginitis.If your vagina feels dry, itchy, or sex is painful, you may have irritation but not an infection. Monitor your symptoms to see if they worsen and use a vaginal moisturizer or personal lubricant for greater comfort during intercourse. You can also try switching to unscented soaps, getting out of wet workout clothes quickly and other tactics to reduce the inflammation and allow the vagina to restore its natural balance.
2. Bacterial Vaginosis.An overgrowth of bacteria in your vagina can lead to an infection called bacterial vaginosis. BV tends to have a grayish-white discharge and a strong fishy odor. BV is easily treated with common antibiotics your doctor can prescribe.
3. Yeast infection.Yes, a yeast infection is a type of vaginitis. Caused by an overgrowth of the fungus candida, yeast infections tend to produce thick, white vaginal discharge that can be clumpy, like cottage cheese. Yeast infections can be treated with over-the-counter anti-fungal creams or see your doctor for an oral pill.
4. Trichomoniasis or Trich.This type of vaginitis is a sexually transmitted infection (STI) caused by a parasite and often produces a yellowish-green or frothy vaginal discharge. Your doctor can diagnose trichomoniasis and treat it with an antibiotic.
5. Chlamydia or Gonorrhea.These are sexually transmitted bacterial infections that only your doctor or sexual health clinic can diagnose and treat with antibiotics.
Is it Bacterial Vaginosis (BV) or a Yeast Infection?
It can be hard to tell what kind of vaginitis you have but determining the cause can help you choose the correct treatment. While yeast infections tend to be more common, see your doctor to find out if something else – like a bacterial infection – is going on.
Because getting a vaginal yeast infection is so common after taking antibiotics, many doctors proactively prescribe an anti-fungal medication you can take if you start having symptoms of vaginitis after finishing your antibiotics.
Help Keep Your Vagina pH Balanced & Moisturized
Mild vaginitis is frequently caused by vaginal dryness or non-infectious changes to your vaginal pH. You can’t prevent every cause of vaginitis, but there are some things you can do to help keep your vagina healthy and reduce inflammation and irritation.
1. Use a vaginal moisturizer. If you experience vaginal dryness due to hormones, medication, or even stress, try using a long-lasting vaginal moisturizer to enhance your lubrication. We recommend Replens Long Lasting Vaginal Moisturizer and Replens Silky Smooth Personal Lubricant.
2. Watch how you wash down there. Avoid heavily perfumed soaps and body washes. Try RepHresh Vaginal Gel to eliminate vaginal odor and maintain a healthy vaginal pH.
3. Take probiotics. Help keep the good bacteria flourishing in your gut and in your vagina with oral probiotics, such as RepHresh™ Pro-B™ Feminine Probiotic Supplement*.



